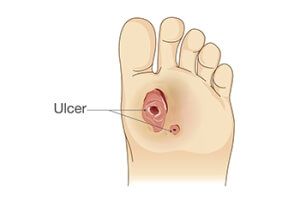
Diabetic Foot Ulcers

A foot ulcer is defined as any break in the skin. It is the most common type of diabetic foot wound and can lead to loss of functioning and severe complications. These foot wounds often result from factors such as poor blood sugar control, diabetic peripheral neuropathy, and abnormal foot mechanics due to deformities. Diabetic peripheral neuropathy, a side effect of diabetes, can also lead to a loss of protective sensation in the feet, making early injury detection challenging. The assessment of the diabetic foot involves a comprehensive foot and body examination. This can consist of assessing risk factors, undergoing a dermatologic and musculoskeletal evaluation, and having neurologic tests that can determine the degree of sensation. Treatment of diabetic foot ulcers includes debridement, wound culturing, and wound dressings. Additionally, it is important to monitor glycemic control and infection control. Their prevention and management are essential to improve the patient’s quality of life. If you have diabetes and have developed a foot wound or any other foot condition, it is strongly suggested that you make an appointment with a podiatrist who can evaluate your situation, and receive the appropriate treatment.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Nrup Tolat, DPM from Atlanta Total Foot & Ankle Care. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
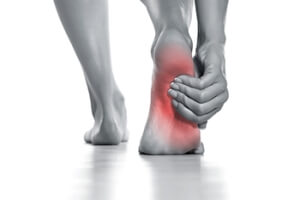
Causes and Effective Remedies for Heel Pain

Heel pain is a common ailment that can disrupt daily life and activities. One of the primary culprits is plantar fasciitis, which occurs when the thick band of tissue known as the plantar fascia becomes inflamed or irritated. The plantar fascia is found on the bottom of the foot, and connects the heel to the toes. Plantar fasciitis often results from overuse, wearing improper footwear, or a sudden increase in physical activity. Another common cause of heel pain is Achilles tendonitis, which affects the Achilles tendon at the back of the heel, usually as a result of excessive strain or overuse. To alleviate heel pain, it is beneficial to rest and elevate the affected foot. Wearing proper footwear with adequate arch support can significantly help, in addition to wearing custom orthotic inserts. Performing stretching exercises for the calf muscles and Achilles tendon also can aid in recovery. In severe cases, surgical intervention may be necessary. If you are experiencing heel pain, it is strongly suggested that you make an appointment with a podiatrist who can determine the cause and offer treatment options that are right for you.
Many people suffer from bouts of heel pain. For more information, contact Nrup Tolat, DPM of Atlanta Total Foot & Ankle Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
Wounds That Don't Heal Need to Be Checked
Fall Proofing the Home for Elderly Loved Ones

As we age, the risk of falls in our homes becomes a growing concern. The good news is that with a few thoughtful modifications, you can transform your living space into a safe haven for elderly family members. This can begin by decluttering walkways, ensuring clear, unobstructed paths, followed by removing tripping hazards such as loose rugs and electrical cords. Installing handrails and grab bars which can provide essential support, is critical in bathrooms and staircases. Adequate lighting is vital, and dimly lit areas can be brightened, in addition to adding nightlights which can reduce the risk of stumbling in the dark. Consider anti-slip flooring options to improve traction. In the bathroom, invest in a shower chair and non-slip mats to prevent accidents. Regular maintenance of your home's infrastructure, including checking for loose floorboards or uneven surfaces, is also important. If you would like additional information about effective methods to keep your home safe for senior family members, it is suggested that you consult with a podiatrist.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Nrup Tolat, DPM from Atlanta Total Foot & Ankle Care. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
Bunion Surgery May Help Provide Pain-Free Feet

Bunions, those painful bony bumps that form at the base of the big toe, can be a source of immense discomfort and self-consciousness. When conservative measures fail to provide relief, bunion surgery may become a viable option. Medically known as a bunionectomy, this surgical procedure aims to correct the misalignment of the big toe joint, eliminating pain and improving foot function. During the surgery, the podiatrist will remove the bony bump and realign the bones and tissues to their proper position. Recovery may take several weeks, during which weight must be kept off the affected foot. It is important to follow post-operative care instructions diligently. While bunion surgery is a significant step, it offers a promising path toward a life free from the pain and inconvenience of bunions, allowing you to walk comfortably and confidently once again. If you have a bunion, it is suggested that you consult with a podiatrist who can determine if surgery is correct for you.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact Nrup Tolat, DPM of Atlanta Total Foot & Ankle Care. Our doctor will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot and Ankle Surgery
When conservative, noninvasive methods prove ineffective, surgery may be selected as the next course of action for the treatment of your foot or ankle condition. A wide number of foot and ankle surgical procedures exist, and it is up to your podiatrist to determine which intervention will be most appropriate and helpful for your case. Some surgical procedures include bunion surgery, fusion, hammertoe surgery, heel spur surgery, metatarsal surgery, nail surgery, neuroma surgery, reconstructive surgery, skin surgery, and tendon surgery. Typically, surgery is turned to as a definitive way to alleviate excessive pain or discomfort and to return your foot to full mobility.
Regardless of the location on the body, all surgical procedures require preoperative testing and examination to ensure the surgery’s success and preferred outcome. A review of your medical history and medical conditions will take place, as will an evaluation of any current diseases, illnesses, allergies, and medications. Tests such as blood studies, urinalyses, EKG, X-rays, and blood flow studies may be ordered. Because the procedure involves the foot and/or ankle, the structures of your feet while walking may also be observed by your podiatrist.
Care post-surgery will depend on the type of surgical procedure performed. Typically, all postoperative care involves rest, ice, compression, and elevation. To improve and ensure a safe recovery, your foot and ankle surgeon may also employ the use of bandages, splints, surgical shoes, casts, crutches, or canes. He will also determine if and when you can bear weight. A timely and thorough recovery is a priority for both you and your podiatrist, and carefully following postoperative instructions can help achieve this.
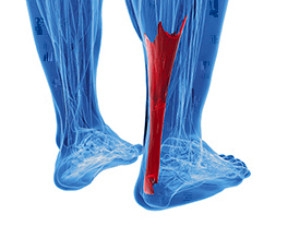
Symptoms Causes and Effective Treatment for an Achilles Tendon Injury

Achilles tendonitis is a painful condition affecting the Achilles tendon which is found at the back of the ankle. Achilles tendinitis is characterized by inflammation and irritation of the Achilles tendon, leading to discomfort during movement. Common symptoms can include pain and stiffness near the heel, often worsening after physical activity. Overuse and repetitive stress are primary culprits, frequently affecting athletes and those who engage in intense physical activities. Having tight calf muscles, wearing improper footwear, and sudden increases in exercise intensity can also contribute to getting an Achilles tendon injury. Managing Achilles tendinitis involves rest, compression, and elevation, along with performing gentle stretching and strengthening exercises. Severe cases may require medical intervention, and it is suggested that you contact a podiatrist who can provide you with an accurate diagnosis and tailor a treatment plan that is right for you.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Nrup Tolat, DPM of Atlanta Total Foot & Ankle Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.